
Partnership & Purpose
Trauma, Domestic Abuse and Health: Bridging Research, Strategy and Frontline Practice
Research over the past few decades has shown clear links between trauma, chronic stress and physical health. The Adverse Childhood Experiences (ACE) Study, conducted by Centers for Disease Control and Prevention and Kaiser Permanente, found that higher levels of childhood adversity are associated with increased risk of a range of health difficulties later in life.
Research also shows that people who have experienced domestic abuse and coercive control have higher rates of long-term health conditions, including chronic pain, digestive disorders, sleep difficulties and other stress-related illness.
These connections are still often missed in practice. Survivors may not always access specialist domestic abuse services and may instead present within health, mental health or substance misuse services, particularly in more complex cases involving disability, chronic illness or long-term trauma.
Greater awareness of the links between trauma, chronic stress and physical health can help professionals recognise these patterns and develop more joined-up responses for survivors whose experiences may otherwise remain hidden within services.
Supporting Trauma-Responsive Practice
This work is grounded in partnership with organisations and professional communities, strengthening trauma-responsive and disability-inclusive practice across domestic abuse and therapeutic services.
Operating at the intersection of strategy and frontline practice, the focus is on ensuring trauma-informed understanding is reflected in everyday work — including safeguarding decisions, team culture, relational safety and the lived experiences of those seeking support.
Training and reflective practice spaces support professionals to explore these complexities and translate trauma awareness into consistent, ethical and responsive practice across sectors.
From Trauma-Informed to Trauma-Responsive

Trauma-informed frameworks represent important and necessary progress. They increase awareness of how trauma affects individuals and systems.
However, awareness alone does not always translate into embodied practice.
Trauma-responsive practice requires a deeper integration, where understanding shapes behaviour, communication, safeguarding decisions and organisational culture. It means recognising survival responses in both service users and staff teams. It involves strengthening relational safety, responding to nervous system dysregulation in real time, and ensuring that policy language is reflected in day-to-day interactions.
Moving from informed to responsive is not about replacing existing frameworks. It is about deepening them, grounding them and supporting teams to translate knowledge into lived, relational and physiologically informed practice.

Strategic Mapping & Systems Development
Over the past three years, I have collaborated on strategic mapping of disability and domestic abuse provision across North Somerset, working in partnership to identify systemic gaps, access barriers and opportunities to strengthen safety and inclusion.
A core focus of this work has been looking at how services and professional communities to move beyond trauma-informed awareness towards trauma-responsive implementation. While trauma-informed frameworks represent important progress, sustainable change requires that understanding is reflected in day-to-day relational practice, safeguarding processes and organisational culture.
This includes strengthening embodied awareness of nervous system responses within teams, embedding disability-inclusive safeguarding approaches, addressing the additional risks faced by those living with chronic health conditions, and ensuring that trauma language translates into genuine safety in practice, not only policy.
Trauma-Responsive Practice & the PNI Model
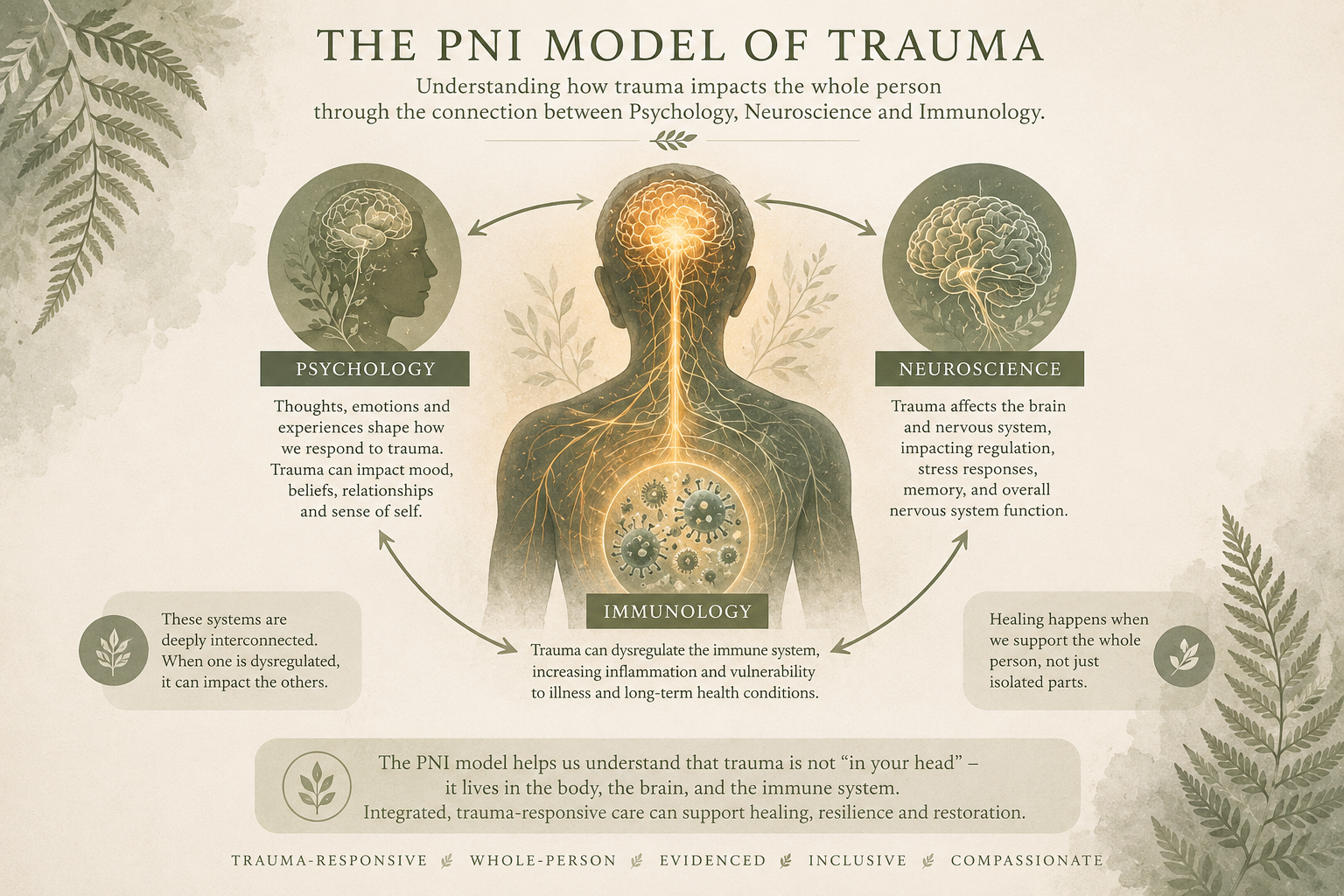
Consultancy and training are underpinned by a Psychoneuroimmunology (PNI)-informed trauma model.
This perspective recognises the interaction between psychological experience, nervous system regulation and immune functioning. Prolonged stress and trauma can influence physiological systems, shaping both individual wellbeing and organisational dynamics.
Bringing a therapeutic trauma lens into strategic work allows for a deeper understanding of:
Survival responses and nervous system activation
The embodied impact of chronic stress
The intersection of trauma, disability and long-term health conditions
How staff regulation and team culture influence service delivery
This framework supports organisations to integrate relational safety and physiological awareness into both frontline practice and systemic development.
Areas of consultancy & training may include:
Collaborative strategic mapping and reflective service review informed by a PNI-based understanding of trauma and chronic stress
Development of trauma-responsive implementation approaches grounded in nervous system awareness and relational safety
Training for staff and leadership teams on trauma, chronic illness and the physiological impact of prolonged stress
Strengthening disability-inclusive and chronic illness-aware safeguarding approaches within domestic abuse settings
Facilitating reflective practice spaces that deepen understanding of survival responses, regulation and the embodied impact of trauma in frontline work
Supporting cross-sector partnership and organisational development that integrates therapeutic trauma perspectives into everyday practice

Invitation to Collaborate
If your organisation is seeking to move beyond awareness towards responsive, embodied and disability-inclusive practice, or if you feel uncertain how to translate trauma-informed principles into consistent frontline response, I welcome a conversation.
Whether you are looking for bespoke training, reflective development spaces or strategic support, we can explore together what would be most helpful for your service.

